GLP-1 Foods to Avoid: 9 Foods That Secretly Block Your Natural GLP-1 Response — Especially for Women

GLP-1 Foods to Avoid: 9 Foods That Secretly Block Your Natural GLP-1 Response — Especially for Women
GLP-1 foods to avoid are just as important as the foods you add — because nine specific foods actively suppress the gut hormone that controls your fullness, and most women eating them have no idea. Here is the research-backed list.
👉 This article is part of our complete guide: Natural GLP-1 Foods That Work Like Ozempic for Women
GLP-1 Foods to Avoid If You Want Better Appetite Control
If you struggle with constant hunger or afternoon cravings, the problem may not only be what you eat — but the GLP-1 foods to avoid that quietly weaken your body’s natural fullness signal. GLP-1 is a hormone that helps control appetite, slow stomach emptying, and signal your brain that you are full. Certain foods can suppress this response, making it harder to feel satisfied after meals. Highly processed snacks, excess alcohol, and refined sugars are some of the most common GLP-1 foods to avoid because they can disrupt gut signaling and reduce the hormone response that keeps hunger in check. Identifying and reducing these foods can help your body maintain stronger appetite control naturally.
At a Glance: The 9 GLP-1 Blockers
| Food | How It Blocks GLP-1 | Women-Specific Risk |
|---|---|---|
| Alcohol | Reduces GLP-1 by 34% acutely in women | Doubles down via estrogen suppression |
| Ultra-processed snack foods | Destroys gut microbiome → collapses SCFA-GLP-1 baseline | Worse in women with PCOS, gut dysbiosis |
| Sugary drinks (soda, juice) | Liquid glucose bypasses distal L cells | Blood sugar crash triggers afternoon cravings |
| White bread and refined grains | Rapid digestion exits GI before distal L cells activate | Amplified during luteal phase |
| Fried foods and trans fats | Gut inflammation impairs L cell function | Worsens insulin resistance → blunts GLP-1 receptors |
| Processed and deli meats | Preservatives and sodium damage gut microbiome | Linked to leptin resistance in women specifically |
| Artificial sweetener-heavy foods | Disrupts gut microbiota balance | Impairs GLP-1 circadian signaling |
| High-sugar breakfast cereals | Spikes and crashes GLP-1 baseline before 9 AM | Destabilizes entire day’s GLP-1 rhythm |
| Excess caffeine | Raises cortisol → glucocorticoids suppress GLP-1 | Perimenopause and stress amplify cortisol load |
Why “Foods That Block GLP-1” Is a Topic Nobody Covers — And Should
Every article on natural GLP-1 tells you what to eat more of. Avocado. Greek yogurt. Beans. Great — all of that is real. But here is what the same articles leave out: certain foods do not just fail to help your GLP-1. They actively block it. They suppress secretion, blunt receptor sensitivity, or systematically destroy the gut microbiome that produces the baseline GLP-1 signal your body runs on every day.
For women, this matters more than most people realize. Your GLP-1 system is more sensitive to hormonal disruption than men’s — the estrogen-GLP-1 connection means that anything raising cortisol, damaging the gut microbiome, or impairing estrogen activity hits your fullness hormone system harder. The nine foods below do exactly that.
(And this is the part that most GLP-1 articles skip entirely.)
Food 1: Alcohol — Reduces GLP-1 by 34% in Women

The research: A placebo-controlled crossover study published in Addiction Biology — specifically conducted in women — measured GLP-1 levels after alcohol consumption (0.5g/kg of fat-free mass) versus placebo. Alcohol decreased GLP-1 by 34% (95% CI, 16%–52%) in both operated and non-operated control women. The researchers concluded that one mechanism behind alcohol’s “apéritif effect” — the well-known phenomenon of alcohol increasing food intake before a meal — is this direct suppression of endogenous GLP-1 and resulting reduction in satiety signaling.
What this means practically: That glass of wine before dinner is not neutral. It is actively lowering the hormone that would otherwise tell you when you have eaten enough. The meal that follows happens with a 34% GLP-1 deficit — which is a physiologically meaningful suppression, not a rounding error.
The women-specific layer: GLP-1 production in women depends partly on estrogen activity. Alcohol disrupts estrogen metabolism — particularly in perimenopause when estrogen is already declining. This adds a second suppression layer: the direct 34% GLP-1 drop from alcohol’s acute effect, plus downstream estrogen disruption that further reduces baseline GLP-1 production. The impact in women is not just equal to men. It is compounded.
The swap: Sparkling water with lime before dinner. Not a perfect substitute — nothing is — but it keeps the ritual without the hormonal cost. If you drink, doing so after eating — rather than before — at least preserves the meal-time GLP-1 signal when it is most needed.
👉 Calculate your accurate TDEE if alcohol is part of your routine — free TDEE Calculator
Food 2: Ultra-Processed Snack Foods — They Collapse Your GLP-1 Baseline

The research: Ultra-processed foods (UPFs) — chips, crackers, packaged cookies, processed snack bars — are characterized by high synthetic additive content, emulsifiers, and near-zero fiber. A 2025 PMC review confirmed that UPFs reduce gut microbial diversity, lower levels of beneficial bacteria including Akkermansia muciniphila and Faecalibacterium prausnitzii, and increase pro-inflammatory organisms.
Why does this matter for GLP-1? Because those gut bacteria produce short-chain fatty acids (SCFAs) — and SCFAs are a primary driver of GLP-1 secretion from gut L cells. A study published in Gut Microbiota journal (2023) confirmed that gut microbiome depletion completely abolished the postprandial GLP-1 response. No healthy gut microbiome. No SCFA production. No baseline GLP-1 signal.
A cross-sectional study of 59 women specifically found that higher UPF consumption was directly associated with leptin resistance and measurable changes in gut microbiota composition — independent of total calorie intake.
The slow damage: This is not an acute effect like alcohol. UPFs do not suppress a single meal’s GLP-1 response. They chip away at the gut microbiome over weeks and months — gradually collapsing the SCFA-driven GLP-1 baseline that your fullness system runs on. Women who eat UPFs regularly are not just making individual poor food choices. They are systematically degrading the biological infrastructure of their GLP-1 system.
The swap: The core principle: if it has more than 5 ingredients and any of them are unrecognizable, it is likely a UPF. Whole food snacks — walnuts, hard-boiled eggs, full-fat Greek yogurt, apple slices with almond butter — protect the gut microbiome rather than eroding it.
Food 3: Sugary Drinks — Liquid Glucose Bypasses Your GLP-1 System
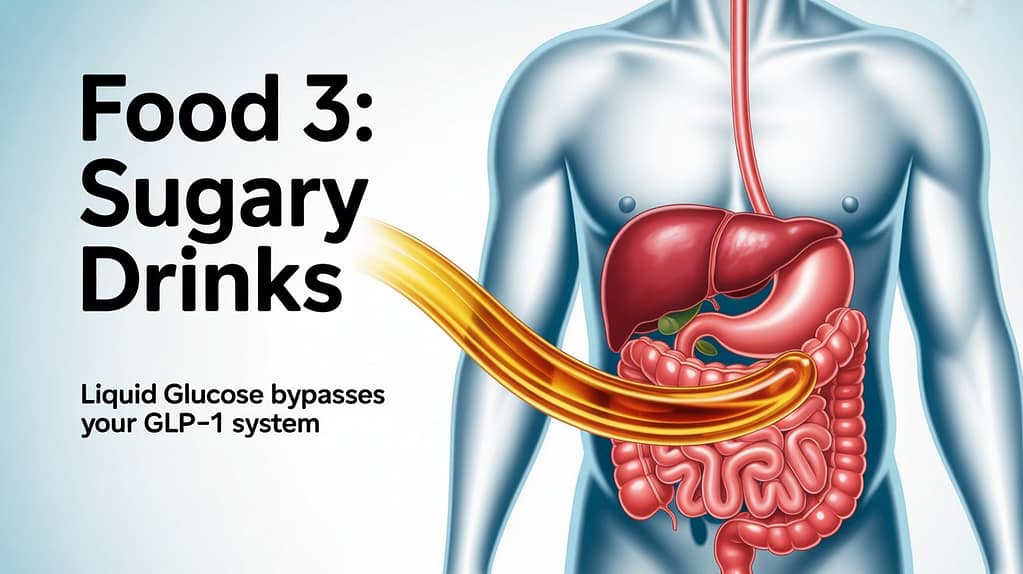
The research: GLP-1 is primarily secreted by L cells located in the distal small intestine and colon. For these cells to receive the signal to release GLP-1, nutrients need to travel far enough down the GI tract to reach them. Liquid glucose — from soda, juice, sports drinks, sweetened coffee drinks — empties from the stomach and absorbs in the upper GI extremely rapidly. It is gone before it reaches the distal L cells that trigger the strongest GLP-1 response.
Solid food, by contrast, slows gastric emptying, ferments in the lower GI, and activates both proximal and distal L cells across a longer time window. Same calories. Dramatically different GLP-1 outcome.
The blood sugar crash cascade: Liquid glucose causes a sharp blood sugar spike — and a sharp spike always precedes a sharp crash. When blood sugar crashes 90–120 minutes after a sugary drink, GLP-1 is not there to cushion the landing. The result: intense carbohydrate cravings at the exact time you thought you were fine because you just had a drink. Most women recognize this pattern (afternoon soda → 3 PM sugar craving) without knowing the hormonal mechanism driving it.
Women-specific note: During the luteal phase (days 15–28), progesterone already reduces GLP-1 sensitivity. Adding sugary drinks on top of a hormonally weaker GLP-1 response during this phase amplifies the hunger-craving cycle significantly.
The swap: Water, sparkling water, unsweetened herbal tea, black coffee (moderate), kefir. If you need something sweet, a piece of whole fruit delivers fructose inside fiber — slowing absorption and partially preserving the distal L cell GLP-1 response.
👉 Track your blood sugar management — free Body Fat and Metabolic Tools
Food 4: White Bread and Refined Grains — The Fast-Digestion GLP-1 Miss

The research: Refined carbohydrates — white bread, white rice, standard pasta, most crackers — are digested and absorbed in the upper small intestine before they reach the L cells in the distal gut. This means they trigger a weak or delayed GLP-1 response compared to the same calories delivered through intact whole grains, legumes, or fiber-rich foods.
The glycemic index research confirms this pattern: high-GI foods (white bread GI ≈ 75) generate faster glucose absorption, weaker GLP-1 signaling, and stronger post-meal blood sugar swings than lower-GI equivalents (sourdough GI ≈ 54, steel-cut oats GI ≈ 55).
This is not about carbohydrates being bad. It is about delivery speed. The same amount of carbohydrate in lentils — which digest slowly and ferment in the lower GI — produces meaningfully more GLP-1 than the same amount in white bread. Structure matters.
The luteal phase amplification: During days 15–28 of the menstrual cycle, GLP-1 sensitivity drops and carbohydrate cravings intensify. Eating refined grains during this window — when your GLP-1 system is already at a disadvantage — maximizes the blood sugar volatility and carbohydrate craving cycle. This is biologically predictable, not a willpower failure.
The swap: Sourdough over white bread (slower fermentation = lower GI). Steel-cut oats over instant oatmeal. Brown rice over white rice. Whole wheat pasta over standard pasta — and eat it after your protein and vegetables, not as the first course.
Food 5: Fried Foods and Trans Fats — Gut Inflammation Impairs L Cell Function
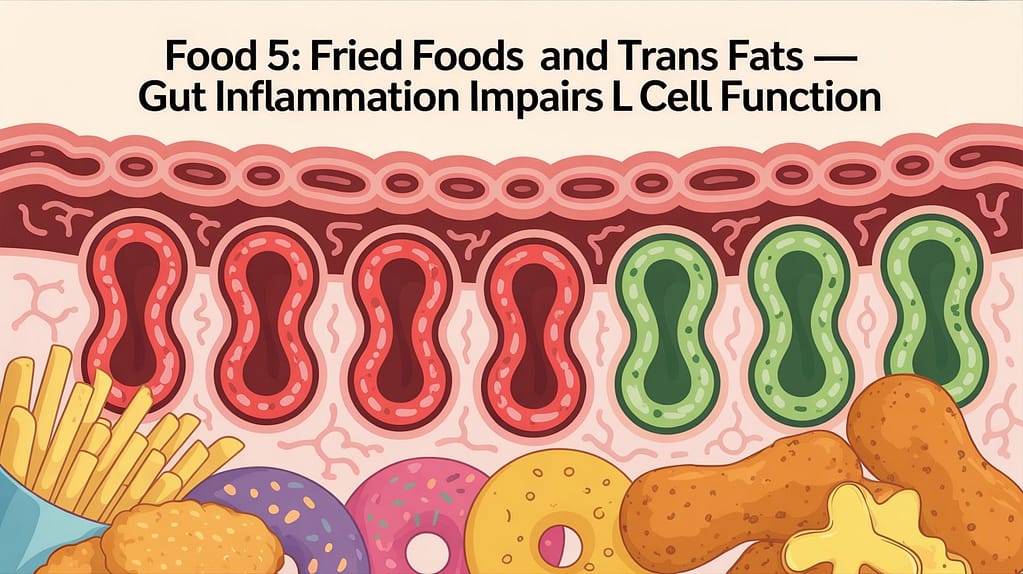
The research: Trans fats (partially hydrogenated oils) and excessive omega-6 fatty acids from repeated frying — found in fast food, fried restaurant food, and some processed snacks — promote gut inflammation through multiple pathways. They increase intestinal permeability, reduce microbial diversity, and trigger pro-inflammatory signaling that directly impairs the function of gut enteroendocrine L cells.
L cells do not operate in isolation. They are embedded in the gut mucosa and are sensitive to the inflammatory environment around them. Chronic gut inflammation from a high-trans-fat, high-omega-6 diet does not just damage the gut barrier — it blunts the L cells’ ability to respond to nutrients and secrete GLP-1. This is not theoretical. PMC studies on high-fat diet models consistently show reduced GLP-1 secretion per gram of food consumed in subjects with gut inflammation versus those without.
The women-specific angle: Inflammation interacts with estrogen. Chronic gut inflammation disrupts the estrogen-GLP-1 axis, which already makes women more vulnerable to GLP-1 suppression than men. Women with endometriosis, PCOS, or chronic inflammatory conditions face compounded GLP-1 dysfunction from fried food consumption.
The swap: Air frying, baking, or sautéing in olive oil (a healthy fat that actually supports GLP-1 — covered in our main foods guide) instead of deep frying. The goal is not eliminating fat. It is replacing inflammatory fats with ones that support rather than suppress GLP-1 function.
Food 6: Processed and Deli Meats — Sodium and Preservatives Hit the Gut Microbiome
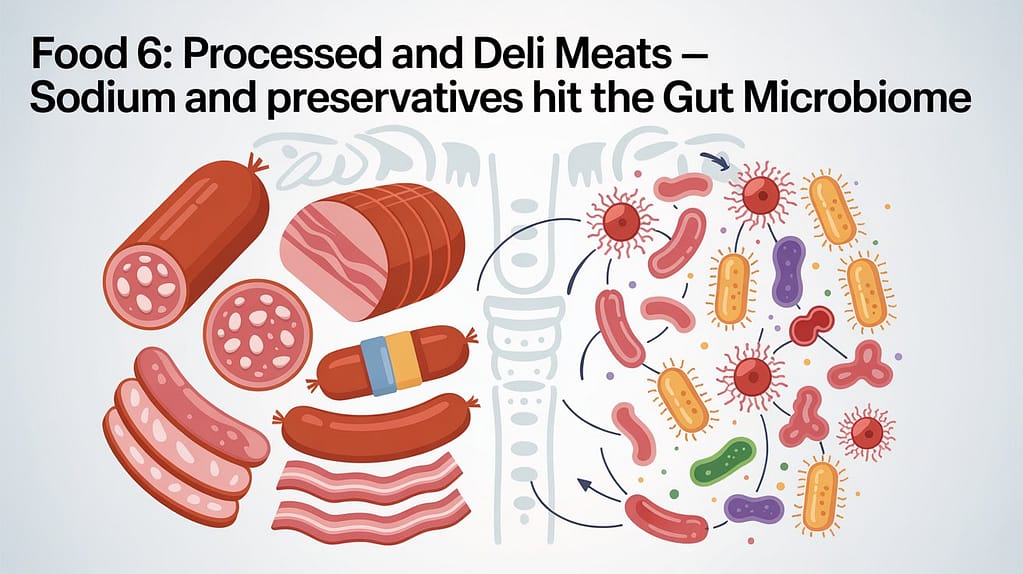
The research: Processed meats — deli turkey, salami, pepperoni, hot dogs, packaged sausages — are UPFs in protein form. They contain sodium nitrates, sodium nitrites, phosphate additives, and other preservatives that research has linked to gut microbiome disruption and increased intestinal inflammation.
The PubMed-published cross-sectional study of 59 women found that ultra-processed food consumption (a category that includes processed meats) was directly associated with leptin resistance and measurable changes in gut microbiota composition. And since GLP-1 baseline production depends on a healthy gut microbiome producing SCFAs — anything damaging that microbiome is indirectly suppressing GLP-1.
Processed meats also typically replace a protein source that would actually help GLP-1. A chicken breast, a hard-boiled egg, or a serving of Greek yogurt delivers protein that directly triggers GLP-1 from gut L cells. A deli turkey sandwich delivers protein wrapped in preservatives that undermine the gut environment those L cells depend on.
The swap: Whole protein sources — rotisserie chicken (without additives), canned wild salmon or tuna, hard-boiled eggs, cottage cheese, or Greek yogurt — at every meal. Protein is non-negotiable for GLP-1 support. Processed protein is not the same as real protein.
Food 7: Artificial Sweetener-Heavy Foods — The Gut Microbiome Disruption Nobody Talks About
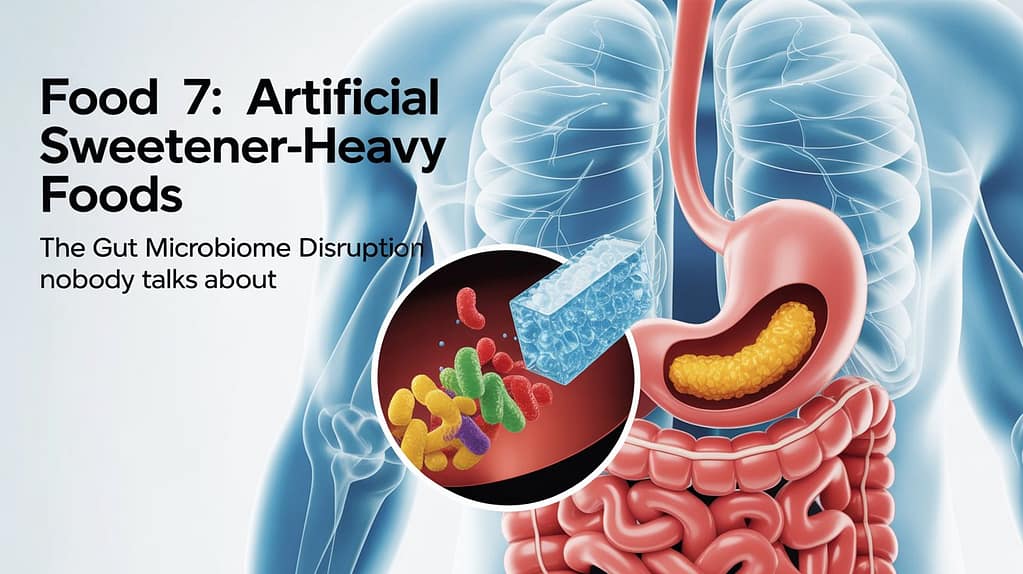
The research: Artificial sweeteners — saccharin, sucralose, aspartame, acesulfame-K — are in thousands of products marketed as “diet,” “zero calorie,” or “sugar-free.” The evidence on their gut microbiome effects is not settled, but the signals are concerning. Studies in both animal models and humans suggest that non-nutritive sweeteners can disrupt the composition and diversity of the gut microbiome — the same microbiome that produces SCFAs and drives baseline GLP-1 production.
A 2022 Nature study found that saccharin and sucralose specifically impaired glucose tolerance in humans — through microbiome-mediated mechanisms. Whether these effects are large enough to clinically impair GLP-1 in all individuals is not yet established. The honest position is: the mechanism is plausible, the evidence is early-stage, and the risk in regular high-consumption is real enough to warrant caution.
The women-specific concern: Women with PCOS already have impaired GLP-1 receptor sensitivity from insulin resistance. Adding gut microbiome disruption from high artificial sweetener consumption on top of this existing deficit compounds the GLP-1 dysfunction.
The nuance: This is not a reason to avoid every diet product forever. A small amount of sucralose in your coffee is a different risk than drinking three diet sodas daily. The issue is habitual high consumption of artificially sweetened products replacing fiber-rich, whole foods.
The swap: If you need sweetness, try naturally lower-calorie options: a small amount of raw honey in oatmeal (which provides some fiber and polyphenols), fresh berries, or cinnamon (which blunts blood sugar spikes through a separate mechanism — research-confirmed).
Food 8: High-Sugar Breakfast Cereals — They Destabilize Your Entire Day’s GLP-1

The research: The first meal of the day sets the GLP-1 hormonal tone for everything that follows. A PubMed study comparing high-protein, high-fat, and high-carbohydrate breakfasts PMID 23666746 found that GLP-1 and PYY (a companion satiety hormone) were highest after the high-protein breakfast — and significantly lower after the high-carbohydrate breakfast — with the differences persisting throughout the morning study period.
High-sugar cereals — most mainstream breakfast cereals, even ones marketed as “healthy whole grain” — have glycemic indexes of 70–83. They spike blood sugar in the 7–9 AM window when GLP-1 is naturally rising with the circadian rhythm. Rather than catching that circadian GLP-1 rise with a protein-anchored meal, a sugary cereal breakfast produces a blood sugar spike, a rapid crash, and a morning hunger spiral that undermines every food choice made before noon.
The morning-sets-the-day mechanism: Ohio State Health confirmed that GLP-1 follows a circadian rhythm — rising in the morning, peaking midday, declining at night. Eating a high-sugar breakfast at the circadian GLP-1 rise is the nutritional equivalent of pouring water on a starting fire. You get a brief GLP-1 spike from the glucose — and then a suppressed, disrupted baseline for the rest of the morning.
The swap: 30–40g protein at breakfast. Greek yogurt + eggs. Cottage cheese + nuts. A 3-egg omelet with black beans. Anything that anchors the morning meal in protein and fiber catches the circadian GLP-1 rise and carries it forward into the day.
(For the full morning GLP-1 strategy, see: Best Time to Eat to Boost GLP-1 Naturally — Circadian Meal Timing for Women)
Food 9: Excess Caffeine — It Raises Cortisol, and Cortisol Suppresses GLP-1
The research: This one needs a precise qualifier — moderate caffeine is not a GLP-1 blocker. The problem is excess caffeine, defined as roughly more than 400mg per day (4 cups of standard coffee), particularly when consumed after noon.
A study published in Clinical Science (Kappe et al., 2015) — PubMed PMID 25853863 — directly demonstrated that glucocorticoid activation in GLP-1-producing cells reduces GLP-1 secretion in response to glucose and fructose. Dexamethasone (a glucocorticoid/cortisol analog) measurably reduced L cell GLP-1 output. The researchers concluded that glucocorticoid excess contributes to disrupted GLP-1 secretion and may help explain why chronic stress is associated with appetite dysregulation.
Caffeine in excess raises cortisol. Elevated cortisol suppresses GLP-1. This is the mechanism.
The women-specific load: Perimenopausal women already have elevated baseline cortisol from declining ovarian hormone production. Women with chronic stress, poor sleep (see Why Poor Sleep Is Wrecking Your GLP-1 Response), or adrenal dysfunction carry more cortisol burden into any given day — which means the marginal cortisol from excess caffeine adds to an already-elevated baseline. The GLP-1 suppression stacks.
The nuance: One or two cups of coffee in the morning is not a GLP-1 blocker. The research points to habitual high consumption — particularly late-in-the-day caffeine (after 12–1 PM) that also disrupts sleep. Disrupted sleep suppresses GLP-1 by an independent pathway. So excess afternoon caffeine hits GLP-1 from both directions: directly via cortisol elevation, and indirectly by fragmenting sleep quality overnight.
The swap: Limit caffeine to 1–2 cups, consumed before noon. If you want something warm in the afternoon: green tea (which contains L-theanine that modulates the cortisol response to caffeine), or herbal tea with no caffeine.
👉 Assess your stress and cortisol levels — free Stress Level Assessment
The Women-Specific GLP-1 Blocker Pattern: Why These 9 Hit Harder for You
Most GLP-1 articles are written from a gender-neutral metabolic perspective. But women’s GLP-1 system operates differently — and that means the 9 foods above have a compounded effect that the same foods would not produce in men.
The estrogen-GLP-1 connection: Estrogen directly enhances GLP-1 secretion from gut L cells. Anything that suppresses estrogen activity — alcohol, chronic inflammation, elevated cortisol — suppresses GLP-1 through this pathway. This chain does not exist in men.
The perimenopause amplification: Women in perimenopause and menopause are already experiencing reduced GLP-1 sensitivity from declining estrogen. The same alcohol that reduces GLP-1 by 34% in younger women may produce larger functional impairment in perimenopausal women because the baseline is already lower.
The PCOS insulin resistance layer: Women with PCOS have impaired GLP-1 receptor sensitivity from insulin resistance. Every food on this list that worsens insulin resistance — refined grains, sugary drinks, fried foods — further blunts GLP-1 receptor function in an already-compromised system.
The luteal phase window: During days 15–28 of the menstrual cycle, GLP-1 sensitivity drops and carbohydrate cravings rise. The foods on this list are exactly what cravings during the luteal phase reach for — refined grains, sugar, alcohol, fried food. The craving and the GLP-1 suppressor are the same food. That cycle is worth understanding.
👉 Check hormonal factors affecting your GLP-1 response — free Hormone and Thyroid Tools
What to Do Instead: The Simple Substitution Framework
You do not need to overhaul your entire diet simultaneously. The highest-leverage changes are:
Highest priority (eliminate or minimize):
- Alcohol before meals — this is the one change with the most immediate, acute GLP-1 protective effect
- Sugary drinks — liquid glucose is the easiest GLP-1 suppressor to remove
- High-sugar breakfast cereals — replace with 30–40g protein breakfast
Medium priority (reduce significantly):
- Ultra-processed snack foods → whole food snacks
- Processed/deli meats → whole protein sources
- Refined grains → whole grain equivalents with intact fiber
Lower priority but still meaningful:
- Fried foods → baked, air-fried, or sautéed equivalents
- Excess caffeine → limit to morning, cut by noon
- Artificial sweeteners → natural alternatives when possible
(For the foods that actually boost your natural GLP-1, read the complete guide: Natural GLP-1 Foods That Work Like Ozempic for Women)
Key Takeaways
- Alcohol reduces GLP-1 by 34% in women — confirmed by a placebo-controlled crossover study in female subjects. The mechanism behind the “apéritif effect” (alcohol before dinner increases food intake) is this direct GLP-1 suppression.
- Ultra-processed foods gradually destroy the gut microbiome SCFA production that drives baseline GLP-1. This is a slow, cumulative damage — not a single-meal effect.
- Sugary drinks bypass the distal gut L cells that produce the strongest GLP-1 signal. Liquid glucose empties too fast to trigger adequate satiety hormone response.
- White bread and refined grains digest in the upper GI before reaching distal L cells — same calorie, significantly weaker GLP-1 response than whole grain equivalents.
- Excess cortisol — from excess caffeine, chronic stress, or poor sleep — directly suppresses GLP-1 secretion from L cells (Kappe et al., PubMed 25853863).
- The estrogen-GLP-1 connection means these 9 foods hit women harder than men — particularly during the luteal phase and perimenopause.
- Highest-leverage first steps: eliminate pre-meal alcohol, swap sugary drinks for water, replace sugary cereal with a 30–40g protein breakfast.
Frequently Asked Questions
Q: Does one glass of wine really suppress GLP-1 that much? The 34% reduction came from a standardized dose (0.5g/kg of fat-free mass) — which is roughly 1–2 standard drinks depending on body weight. So yes, a single moderate drinking occasion produces measurable GLP-1 suppression in women. The clinical significance of a single occasional glass is smaller than chronic daily drinking — but the mechanism is the same and the effect is real.
Q: Are all artificial sweeteners equally problematic for GLP-1? The evidence is not uniform across all sweeteners. Saccharin and sucralose have the most published human evidence for gut microbiome disruption. Stevia appears to have a more neutral gut microbiome profile in available research. Erythritol and allulose have been shown in studies to actually stimulate modest GLP-1 secretion. The honest answer: the category requires nuance, and the current evidence warrants reducing high-volume habitual consumption, particularly of saccharin, sucralose, and aspartame.
Q: Can you rebuild gut microbiome after eating ultra-processed foods? Yes — the gut microbiome responds to dietary changes within days to weeks. Increasing fiber from legumes, vegetables, and whole grains, combined with eliminating UPFs, measurably shifts microbiome composition toward SCFA-producing species within 2–4 weeks in most human intervention studies. The damage is not permanent. But it is ongoing if the diet does not change.
Q: What about diet soda specifically — does it block GLP-1? Diet soda combines two potential GLP-1 disruptors: artificial sweeteners (particularly sucralose and aspartame in most formulations) and carbonation that can accelerate gastric emptying. The direct evidence on diet soda and GLP-1 specifically in women is limited. The gut microbiome disruption concern is the stronger evidence-based reason to reduce it.
Q: Is coffee actually bad for GLP-1? Moderate coffee consumption — 1–2 cups in the morning — is not a GLP-1 blocker and may have some modest GLP-1-supportive effects through polyphenol pathways. The concern is excess caffeine (>400mg/day) and afternoon consumption that disrupts sleep quality. If your coffee habit stays at 1–2 cups before noon, it is unlikely to meaningfully suppress GLP-1.
Read More in This Series
- 👉 The complete guide: Natural GLP-1 Foods That Work Like Ozempic for Women
- 👉 Sleep and GLP-1: Why Poor Sleep Is Wrecking Your GLP-1 Response
- 👉 Exercise and GLP-1: Which Exercise Boosts GLP-1 the Most for Women
- 👉 Meal timing and GLP-1: Best Time to Eat to Boost GLP-1 Naturally — Circadian Meal Timing for Women
Free Calculators
👉 TDEE Calculator — your daily calorie needs adjusted for activity 👉 BMR Calculator — metabolic baseline to understand your GLP-1 diet targets 👉 Protein Calculator — protein intake to compensate when GLP-1 foods are reduced 👉 Hormone and Thyroid Tools — hormonal factors compounding your GLP-1 suppression 👉 Stress Level Assessment — cortisol-GLP-1 connection assessment
Research Sources: • Addiction Biology — Alcohol Decreases GLP-1 by 34% in Women: Placebo-Controlled Crossover Study (Tremblay et al., 2024) • PMC — Ultra-Processed Foods Destroy Gut Microbiome and Reduce SCFA Production, Impairing GLP-1 (PMC11901572, 2025) • PubMed — Differences in Gut Microbiota of Women by Ultra-Processed Food Consumption (PMID 36411218) • Gut Microbiota — Gut Microbiome Depletion Completely Abolishes Postprandial GLP-1 Response via Bile Acid-TGR5 Signaling (2023) • PubMed — Glucocorticoids Suppress GLP-1 Secretion: Cortisol Reduces L Cell GLP-1 Output (PMID 25853863) • PubMed — High-Protein Breakfast Produces Highest GLP-1 Levels vs High-Carbohydrate Breakfast (PMID 23666746) • Ohio State Health — GLP-1 Follows a Circadian Rhythm, Higher Daytime and Evening • PMC — Crosstalk Between GLP-1 and Gut Microbiota in Metabolic Disease (PMC10790698)



Leave a Reply